Haluks (hallux, halluks, hallux valgus) is a degenerative disease whose symptom is foot deformity. Haluksy occur mainly in women (valgus has almost half of them), and contribute to this include overweight, wearing high heels, standing lifestyle and flat feet.
If you have halluxes, then you need to know that conservative treatment is not always enough, surgery is often necessary.
Haluks ( hallux valgus, hallux, hallux ) is a condition in which the largest toe begins to be crooked and deflects towards the outer edge of the foot, and the metatarsal bone deflects towards the inner edge of the foot.
It is estimated that approximately 100,000 people have hallux in our society. They hinder the functioning and cause great pain and difficulty walking. This problem mainly affects women (this is related to the weaker ligament apparatus of the female foot), but sometimes it is also found in children.
Cure hallux naturally, join yoga teacher training in India from YTTI Rishikesh.

Table of Contents
- How are hallux formed?
- Hallux: symptoms
- Causes of Hallux
- Hallux: the genetic tendency to hallux valgus
- Hallux: how to prevent finger deformation
- How are hallux treated?
- Hallux: when surgery is needed
How are hallux formed?
A high heel overloads the forefoot (forefoot, and shoes with a sharp toe increase the pressure on the toe and transverse arch of the foot, which leads to:
- finger deformation
- development of transverse flatfoot,
- pain.
Under the influence of deformations, the foot begins to work differently: the weight of the body is unevenly distributed, the toe ceases to be a strong support point during walking, the strength of the structures that stabilize the foot deteriorates, the muscles become weaker, and the inner edge of the foot is overloaded.
Hallux: symptoms
Incorrect finger positioning is accompanied by joint lesions in the form of a painful, often inflamed swelling at the base of the finger, on the inside of the foot.
If patients delay the visit to the doctor, deformity and pain may already be advanced, patients have problems buying shoes (pressure on the deformed toe intensifies the symptoms and causes inflammation around the head and bones of the metatarsal and redness and pain).
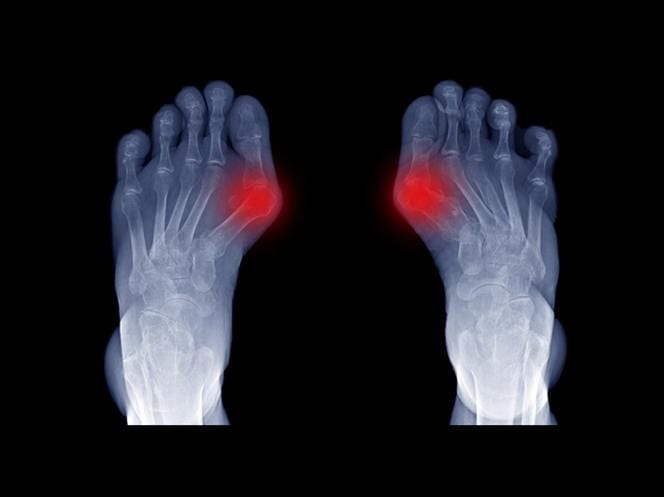
Symptoms that accompany halux may also be:
- exudative bursitis at the height of the metatarsophalangeal joint,
- a bursa (a bag filled with mucus at the friction site on the protruding bone at the toe),
- aching thickenings of the epidermis, which are a response to pressure,
- gradually subluxation of the metatarsophalangeal joint.
Hallux: causes
Formation of the finger and joint degeneration is favoured by:
- wearing uncomfortable, poorly selected footwear (especially high heels and narrow toes),
- overweight,
- avoiding traffic
- standing lifestyle
- Egyptian foot shape (toe longer than the other toe),
- injuries,
- genetic predisposition.
- longitudinal flat feet.
Hallux: the genetic tendency to hallux valgus
The fact that genetic predisposition is most important in the formation of hallux valgus is evidenced by the fact that in approximately 70 per cent in cases it occurs in the female line (grandmother, daughter, granddaughter has it).
We inherit, for example, the incorrect shape of the metatarsal joint surface, connective tissue flaccidity greater than in the statistical population, specific alignment of the metatarsal bones or the so-called Egyptian foot shape.
Hallux: how to prevent finger deformation
The most important thing in preventing the formation of halux is to wear comfortable footwear: not too tight and not too narrow (pointed toes and narrow tips are not allowed), toe exercises, to give up high heels, prevent overweight (a healthy diet) and regular exercise.
How are halux treated?
After the first signs of valgus appear, you should start acting quickly – first of all, go to an orthopaedic consultation.
The doctor will examine your foot and choose the best method for the patient to prevent hallux: orthopaedic insoles, corrective gymnastics or physical therapy.
The simplest treatments for halux that patients have access to are:
- patches for halux or gel shields for halux – often enriched with oils with healing effects, protecting the sore spot;
- interdigital wedges, separators – restore the correct positioning of the toes of the feet, reduce pain and friction, especially recommended in the presence of halux and overlapping fingers or fingerprints in the initial phase of deformation;
- pelottes (pelota – droplet, pillow, drop-shaped insert) gel, T-shaped pelottes, inserts and half-insoles – have a good effect on the pressure distribution in the foot, prevent transverse flatfoot and slow down the development of hallux valgus, you can also use them when wearing shoes on high heels;
- forefoot protection pads – specially designed for ladies who wear high heels,
silicone metatarsal insoles – intended especially for women with transverse flatfoot and halux; due to the current pelott, the transverse arch of the foot is raised, thanks to which the valgus of the hallux valgus is corrected; - band for hallux – the gel liner protects against abrasions and keeps the toe in the correct position, has a positive effect on the distribution of pressure on the foot and prevents muscle weakness and bone deformation;
- correction devices for day or night – effective both in the prevention and treatment of halux and in rehabilitation after surgery. These devices effectively endure pain and inhibit the deepening of deformation;
- Hallufix – splint recommended for the prevention and treatment of halux in the initial phase, with slight deformation, as well as for bursitis and postoperative rehabilitation. This dynamic rail can be used without problems during the day and is an alternative to a rigid rail limiting movement, corrects transverse flat feet.
If the deformities of the fingers begin to be accompanied by pain, the doctor may recommend the use of painkillers and anti-inflammatory drugs. If the pain and distortion are significant and the inoperative (conservative) methods are ineffective, surgery is necessary.
Halux: when surgery is needed
The type of surgical technique used depends on the degree of deformation of the big toe and other foot elements. The multitude of existing operational methods shows that there is no single good and universal method. Therefore, the condition for a good postoperative result is a careful selection of the type of surgery to the degree of deformation of the foot.
The following operational methods are used for haluxes :
- correction only on soft tissues, i.e. joint capsule and tendons with partial head resection of the metatarsal bone in cases of the not very advanced defect;
- Chevron osteotomy – a type of osteotomy performed in some cases of hallux valgus. Osteotomy is performed on the head and metatarsal bones;
- wedge-shaped and hemispherical osteotomies – performed for hallux valgus involving the excision of a bone wedge within the bone and its possible removal or displacement to a different place to correct deformation.
- Scarf method – gives the possibility of early operational loading of the limb and stable anastomosis of fractures allowing for gypsum-free treatment. Patients in a very short time after surgery (2-3 days) can weight the foot by using postoperative shoes (for walking). After not less than 6 weeks, patients return to walking in everyday shoes.
Gypsum-free treatment is also possible in the case of good and stable anastomosis of bone fragments with Kirschner wires after wedge or semi-circular osteotomy. Such an anastomosis is as valuable as the screws in the Scarf method, and the anastomosis material can be easily removed without the need for another operation.
Full loading of the foot before the bone union is achieved, i.e. within six weeks, even with bolting (Scarf or Chevron method) is risky due to the possibility of pulling the bolts out of the bone.
Haluksy – what are they, what causes them?
Haluks is the Latin name for the big toe. This is commonly known as the hallux valgus, i.e. the deformation of the big toe. This disease not only causes aesthetic discomfort but also gives pain and definitely interferes with walking.
What causes haluxes? What are the first symptoms of halux? And can the formation of haluxes be prevented? Our expert Joanna Stodolna-Tukendorf, a physiotherapist, a podologist at the Footmedica clinic, answers these and many other questions.
Haluksy – methods of treatment
Feet can tell a lot about a person, his health, ailments and lifestyle. If they are neglected and distorted, they not only look unsightly but also hurt.
How to avoid the problem of halux and how to cope when they appear? Listen to our expert Joanna Stodolna-Tukendorf, a physiotherapist, podologist at the FootMedica Clinic.
Apart from this, if you are interested to know more about Five Common Heart Diseases then visit our Health category.

